CMT2A Guide: Symptoms, Causes and Treatments
Understanding CMT2A
Charcot-Marie-Tooth disease type 2A is a form of CMT inherited in an autosomal dominant manner. This means that you can inherit the disease from either parent if they also have the disease. However, it is important to remember that around 10% of CMT cases are “sporadic,” meaning that rather than being inherited from either of their parents, these individuals had the genetic mutation occur spontaneously during their embryonic development.
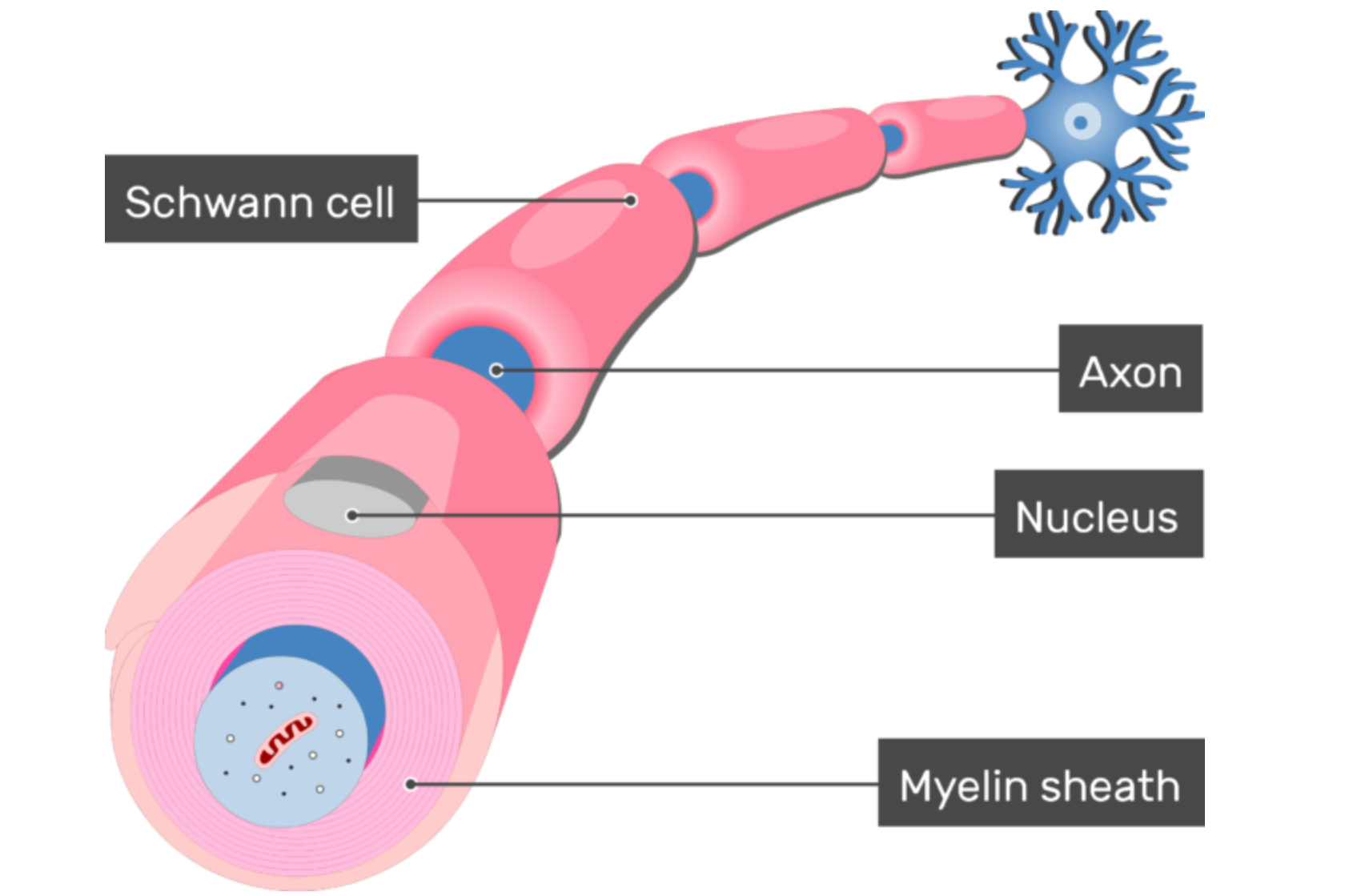
CMT2A is caused by mutations in a gene called MFN2, which produces the protein mitofusin-2. As a type 2 CMT, CMT2A is characterized by dysfunction of axons — the parts of the nerves that are responsible for carrying electrical signals to and from the body and central nervous system (brain and spinal cord). However, people with CMT2A usually have a more severe form, with an earlier age of onset, than people with other CMT2 subtypes.
CMT2A patients account for about 3% of all CMT patients and around 20% of CMT2 patients, making it the most common form of CMT2. Consequently, it is also one of the most common forms of CMT overall.
Causes and Symptoms of CMT2A
The genetic cause of CMT2A is a disease-causing alteration, or mutation, in the gene MFN2. There are many known mutations in MFN2 that cause CMT2A. The MFN2 gene contains the instructions for producing the mitofusin-2 protein, an important component of small structures called mitochondria (singular: mitochondrion) that are found within cells. Mitochondria are the energy factories of every cell — think of them like a power plant. Neurons, which give rise to the axons, have a high demand for energy, and their axons can stretch for long distances. For example, the neurons that control the movement of your toes have axons that stretch from the base of your spine all the way to your toes: a meter-long cell! This means that healthy mitochondrial function and a good distribution of mitochondria throughout neurons are critical for overall neuronal health. When the MFN2 gene is mutated, mitochondrial function is compromised and neurons in the peripheral nervous system become sick. Exactly how the mitochondria dysfunction and causes of disease symptoms are not fully understood yet.
Individuals with CMT2A tend to develop disease symptoms at a young age and demonstrate significant loss of muscle control in their lower limbs during childhood, typically being unable to walk independently by 21 years of age. The disease worsens over time as symptoms progress up the legs toward the torso; a similar progression of weakness is seen in the upper limbs, beginning with the hands. Most people with CMT also experience some loss of or changes in sensation, because the peripheral nerves carry sensory information in addition to movement signals. Some people with CMT2A will also have disease symptoms that indicate abnormalities with certain areas of their central nervous system. These can include a thinning of the spinal cord, inner-ear based hearing loss, or a deterioration of the nerves connecting the retina in the back of the eye to the areas of the brain responsible for vision.
Read more about CMT signs and symptoms
Treatments for CMT2A
While there is no cure for CMT2A, there are several promising therapeutic targets, including molecules to improve overall mitochondrial health or drugs targeting the mitofusin-2 protein directly to diminish the effects of its dysfunction. Additionally, there is the new technology of gene therapy that could lead to promising new avenues of therapeutic intervention.
The CMT Research Foundation is funding multiple projects for various forms of CMT.
Bombelli, F., Stojkovic, T., Dubourg, O., Echaniz-Laguna, A., Tardieu, S., Larcher, K., … Leguern, E. (2014). Charcot-Marie-Tooth Disease Type 2A. JAMA Neurology, 71(8), 1036. https://doi.org/10.1001/jamaneurol.2014.629
Dorn, G. W. (2020). Mitofusin 2 Dysfunction and Disease in Mice and Men. Frontiers in Physiology, 11(July), 1–9. https://doi.org/10.3389/fphys.2020.00782
Feely, S. M. E., Laura, M., Siskind, C. E., Sottile, S., Davis, M., Gibbons, V. S., … Shy, M. E. (2011). MFN2 mutations cause severe phenotypes in most patients with CMT2A. Neurology, 76(20), 1690–1696. https://doi.org/10.1212/WNL.0b013e31821a441e
Morena, J., Gupta, A., & Hoyle, J. C. (2019). Charcot-Marie-Tooth: From Molecules to Therapy. International Journal of Molecular Sciences, 20(14). https://doi.org/10.3390/ijms20143419
Saporta, A. S. D., Sottile, S. L., Miller, L. J., Feely, S. M. E., Siskind, C. E., & Shy, M. E. (2011). Charcot-marie-tooth disease subtypes and genetic testing strategies. Annals of Neurology, 69(1), 22–33. https://doi.org/10.1002/ana.22166
