What Is HNPP Disease: A Guide To Symptoms & Treatments
Understanding HNPP: Hereditary Neuropathy with Liability to Pressure Palsies
Charcot-Marie-Tooth disease encompasses many different subtypes grouped into many different classifications. Most subtypes have “CMT” in their name, but some do not, such as Hereditary Neuropathy with Liability to Pressure Palsies—a CMT subtype classified with CMT1.
HNPP is caused by various mutations in the PMP22 gene. This gene is responsible for instructing Schwann cells to make peripheral nerve myelin. The peripheral nerves are all the nerves that lie outside of the brain and spinal cord—except for the optic nerves—and connect the brain and spinal cord to the rest of the body. These nerves control muscle movement and touch sensations signals (temperature, pain, etc.).
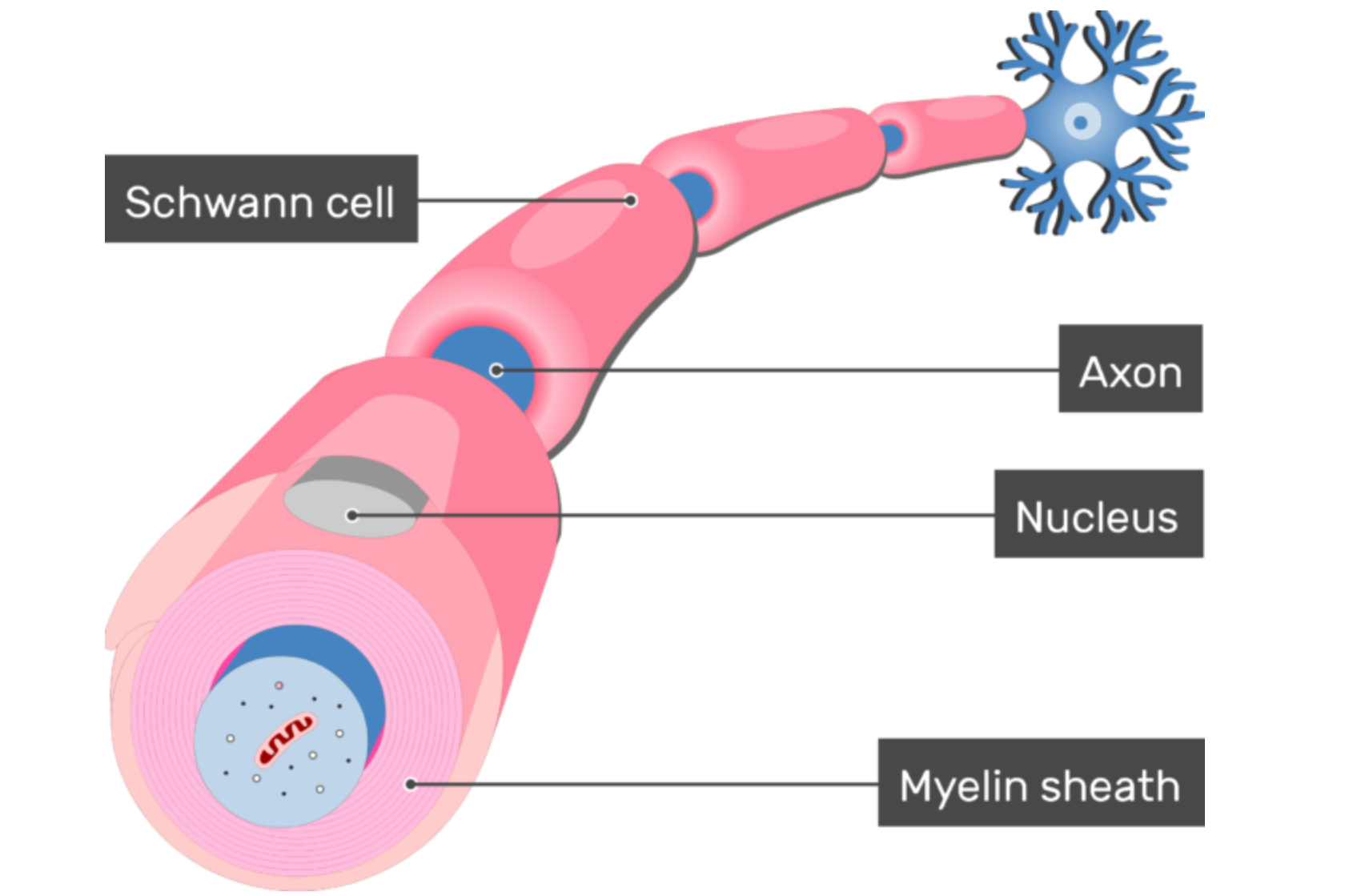
The peripheral nerves are a lot like electrical wire, with two basic components: a metal wire inside and a protective sheath on the outside. The part of the peripheral nerve that transmits a signal (the metal) is the axon. The outer sheath that protects the axon is peripheral nerve myelin. The gene mutations that cause HNPP cause this peripheral nerve myelin to malfunction.
We normally have two copies of the PMP22 gene. The common cause of HNPP is a deletion of one copy of this gene. Most who have HNPP have only one copy of the PMP22 gene instead of the normal two copies. Having only one copy of this gene causes Schwann cells to malform peripheral nerve myelin. Over time, as HNPP progresses, the peripheral nerves start to lose their protective myelin sheath. (Additionally, rare cases of HNPP are caused by a mutation within the PMP22 gene, referred to as a “point mutation” rather than by a deletion of one copy of this gene.)
Symptoms of HNPP
The symptoms of HNPP aren’t too different from the common symptoms of CMT in general. CMT patients who have HNPP also experience both muscle weakness and sensory loss. HNPP is generally not clinically distinguishable from other CMT subtypes.
HNPP symptom onset can start at any time, but usually show up by the time the patient is 30 years old. Symptoms such as numbness, tingling, and muscle weakness are common, just as in CMT in general. However, HNPP symptoms can be episodic and localized to a certain area of the body – the only CMT subtype with this episodic nature.
In HNPP, the most affected areas of the body are the legs, feet, elbows, wrists, or hands. Leaning against hard objects/sharp corners, wearing tight gloves, wearing tight socks, etc., can exacerbate symptoms/trigger an episode. Patients who have HNPP have to be careful to not wear clothes that are too tight, not to wear shoes that are too tight, and if using AFOs, the orthotist must be careful to not create pressure points with the AFOs. Due to the type of abnormality present in the peripheral nerve myelin with HNPP, the peripheral nerves are sensitive to pressure/compression and can be easily injured resulting in a pressure palsy. A pressure palsy is an injury to a nerve caused by pressure or compression and can lead to numbness, weakness, muscle atrophy, and even paralysis of the muscle controlled by the affected peripheral nerve. Sleeping on a mattress that is too firm can create a pressure point in the shoulder, elbow, hip, etc., too, leading to a triggered episode. Stretching improperly can also trigger an episode.
HNPP episodes sometimes resolve in hours but can also last for days, weeks, or months. Sometimes, the palsy can become permanent. Symptom severity varies with each episode depending on which nerve(s) are affected—a motor nerve or a sensory nerve, or both. Typically, symptoms fully resolve in time as the nerve heals from the pressure/compression injury. Usually, when the pressure/compression injury becomes permanent in HNPP, the symptoms tend to be mild, but they can sometimes be severe and debilitating. True to CMT, there’s no reasonable way to predict the severity nor duration of an episode.
Diagnosing HNPP is just like diagnosing any other Charcot-Marie-Tooth disease subtype. Typically, a doctor uses a combination of clinical evaluation, genetic testing, and nerve conduction studies. CMT1 is the CMT classification for demyelinating CMT subtypes that are autosomal dominant in inheritance. Autosomal means the gene with the CMT-causing mutation lives on a numbered chromosome (1-22) and there needs to be only one mutation in the gene to cause CMT. Before the patient’s genetic cause is known, doctors clinically diagnose CMT as CMT1 or CMT2 based on nerve conduction study results. If conduction speeds are slower than 38 meters/second, the clinical diagnosis is usually CMT1; and if faster than 38 meters/second, which is consistent with axonal CMT, the clinical diagnosis is CMT2. Then, should genetic testing result in a conformation, the diagnosis transitions to the subtype related to the identified CMT-causing mutation. Hence, a clinical CMT1 diagnosis becoming an HNPP diagnosis.
Read more about CMT signs and symptoms
Treatments for HNPP
Much like Charcot-Marie-Tooth disease in general, treatment for HNPP focuses on managing symptoms, and may include physical therapy, occupational therapy, and pain management. In severe cases, surgery may be necessary to relieve pressure on affected nerves. Treatment and symptom management is highly individualized to the patient’s needs.
Can You Have HNPP if Neither Parent Did?
Yes, you can have HNPP even if neither parent did. HNPP is inheritable. It’s inheritable because the gene mutations that cause HNPP might be passed onto each of your children when you have HNPP. However, you do not have to have inherited HNPP to have it. When you have HNPP without any family history of the disease, it is caused by a mutation that occurred at or shortly after conception rather than being inherited. When this happens, your HNPP is called a de novo case, or what is a new case that was not inherited. A de novo HNPP case has the same chance of being passed onto your children as though it had been inherited from a parent.
